by Katie Steider, MPH, CPH
(reprinted from NC SHARPPS Program Newsletter)
Phase 2 of the revised Medicare and Medicaid requirements for participation for long-term care facilities (LTCFs) (42 CFR part 483, subpart B) went into effect November 28, 2017. These requirements include the minimum health and safety standards that LTCFs must meet to participate in Medicaid and Medicare. Phase 2 revisions include the requirement for LTCFs to communicate specific information to a receiving provider (e.g. at an acute care hospital) when a resident is transferred or discharged (§483.15(c)(2)). Although the revisions are specific to LTCFs, hospitals should also be aware of the new requirements as they may see changes in communication from LTCFs. These revisions are an opportunity for all healthcare facilities to evaluate their existing interfacility communication methods to assess the information that is included.
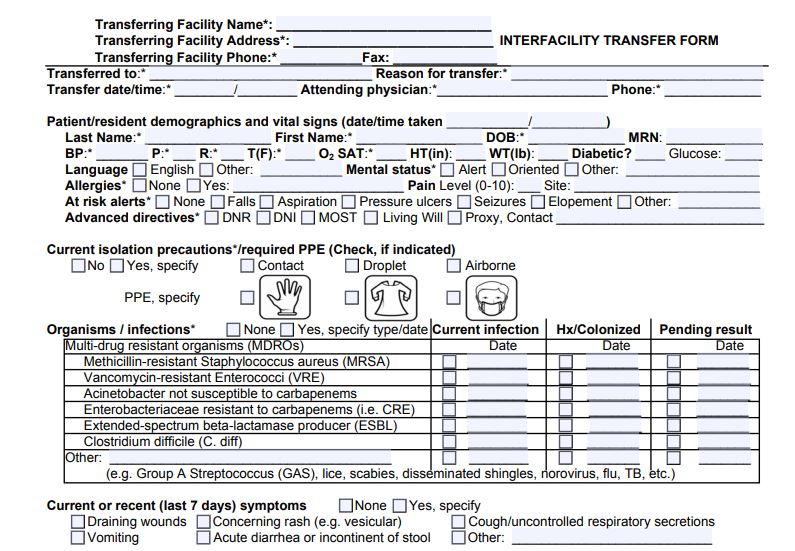
The LTCF requirement for interfacility communication includes, but is not limited to, isolation precaution information due to current or previous infection/colonization, most recent relevant labs, medications (including when last received), advance directive information, and comprehensive care plan goals. In order to facilitate this communication between healthcare settings, the NC Division of Public Health Surveillance for Healthcare Associated and Resistant Pathogens Patient Safety (SHARPPS) Program developed and piloted an interfacility transfer form. The form contains the information necessary for LTCFs to be in compliance with the revised Medicare and Medicaid requirements as they relate to communication to a receiving provider at transfer and discharge.
Pilot participants from an acute care hospital, emergency medical services, and LTCFs reviewed the form favorably. Participants reported the form was useful for identifying individuals on isolation precautions and identifying appropriate personal protective equipment (PPE); initiating isolation precautions in the emergency department; preparing PPE in the ambulance; and identifying individual needs and baseline status. Participants also reported that using a standard interfacility transfer form county-wide was beneficial in communicating information clearly and efficiently between different healthcare facilities. This collaborative approach to interfacility communication reflects CDC recommendations for managing multidrug-resistant organisms in healthcare settings and combating antibiotic resistance. The NC SHARPPS Program encourages any efforts to standardize interfacility communication between healthcare facilities and collaboration to contain and prevent multidrug-resistant organisms.
The interfacility transfer form and instructions are available free of charge from the NC SHARPPS Program webpage. Please email nchai@dhhs.nc.gov with questions or for more information.